Peripheral Artery Diseases

Arteries can be expressed in the simplest terms as the pipe system that carries the blood pumped from the heart. Organs and tissues are nourished by the oxygen they receive from the blood carried by the arteries. Arteries that go to all organs and tissues in the brain, lungs, arms, muscles, legs, skin and abdomen other than the heart are called peripheral arteries.
What are Peripheral Artery Diseases?
The arterial branches that come out of the aorta and carry clean blood to the head, arms, legs and organs and the vein branches that connect to the main vein in order to take the dirty blood coming from them to the heart are called peripheral vessels. Conditions that occur due to various reasons in these vessels and restrict or prevent blood flow are considered within the scope of peripheral vascular diseases.
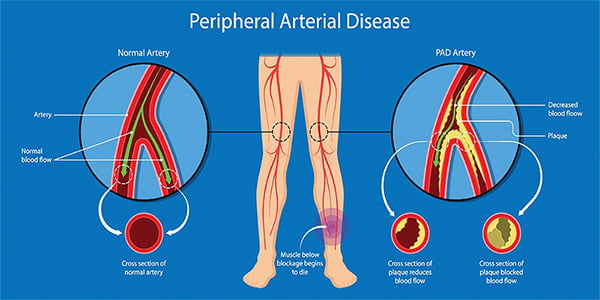
Plaque formations caused by atherosclerosis in the arteries carrying blood to the head, arms, legs and organs cause peripheral arterial diseases. Fat, calcium, cholesterol, fibrous tissue, and other substances in the blood form plaques known as atherosclerosis.
Peripheral arterial disease, which has the risk of affecting all arteries, most often occurs in the arteries leading to the legs. Restriction of blood flow through the narrowed artery due to plaque formations may cause pain in the affected areas.
Atherosclerosis is the main cause of peripheral arterial disease. Factors such as inflammation, rheumatic diseases, various vascular injuries and immune system diseases can accelerate this process.
The progression process of peripheral arterial disease may vary according to many different factors such as the location of the plaque, the patient’s family history, lifestyle habits, and other systemic diseases of the patient. Accordingly, it can be stated that the risk factors that cause atherosclerosis also prepare the ground for the formation of peripheral arteries.
Peripheral Artery Disease Symptoms
Peripheral arterial disease does not cause any symptoms in patients in the initial stage. If the narrowing in the artery increases and accordingly, a critical decrease in blood flow begins, the tissues that cannot receive enough blood die.
In case of disease in the leg arteries, leg pains and cramps due to effort called claudication are frequently encountered. A feeling of heaviness in the legs and painful cramps in the calves or hips after activities such as walking or climbing stairs are considered a sign of narrowing of the leg arteries. The degree of narrowing has a direct effect on the severity of symptoms.
In case of widespread disease of the veins, coldness, bruising, chills, non-healing wounds and even tissue death that may cause limb loss may occur due to ischemia.
How Is Peripheral Artery Disease Treated?
The first step in the treatment of peripheral arterial disease is to quit this habit if the patient is a smoker. Quitting smoking and following a balanced diet are effective in reducing blood cholesterol and other fat levels and keeping blood pressure under control. Accordingly, in the initial stages of peripheral arterial disease, changes in the patient’s lifestyle habits and medical treatment are generally preferred.
In addition, if the patient has diabetes, it should be controlled and regular exercise should be done. Exercise not only helps the muscles to use oxygen more effectively, but also accelerates the development of collateral circulation.
In cases of advanced peripheral arterial disease, interventional or surgical procedures should be used to avoid tissue damage.
- Angioplasty/Stent: Angioplasty, which is less invasive than open surgery, is considered the most effective method for occlusions in large arteries. A catheter is placed over the artery by entering through the arm or groin, and a balloon is sent to the stenosis area. Expansion of the vein is provided by inflating and deflating the area several times. The procedure is completed by placing a small metal mesh tube, known as a stent, to maintain the width.
- Bypass Surgery: By using a vein or a synthetic vessel known as a graft, taken from a different part of the body, blood flow is provided beyond the narrowing or occluded part.
- Endarterectomy: As part of the procedure applied by making an incision on the clogged area in the artery, the piece of plaque causing the obstruction is removed. Thus, blood flow can be corrected.
Peripheral Artery Risk Factors
Pain in the chest during exercise or intermittent leg pain with walking indicates that the tissue’s increased need for blood and oxygen cannot be met. Stroke and heart attack are also considered as examples of sudden oxygen deficiency and malnutrition in tissues due to blood clots completely blocking the arteries.
Although rare, poorly healing open wounds, gangrene, ulcers and some damage may occur due to the decrease in blood flow to the arms or legs as a result of peripheral arterial disease. In these areas that do not receive enough blood, the risk of developing an infection is high. In advanced cases, amputation may become necessary to excise the gangrenous tissue.
Known risk factors for peripheral vascular disease are the same as atherosclerosis and can be listed as follows:
- High levels of LDL cholesterol and triglycerides in the blood;
- Low HDL cholesterol level in the blood;
- Smoking;
- Diabetes;
- History of hypertension of the patient or family;
- The patient’s family history of disease related to atherosclerosis;
- Excess weight.
Who Gets Peripheral Artery Disease?
The incidence of peripheral arterial disease is higher in people with a family history of this disease. And also, other factors that cause peripheral arterial disease to occur frequently are as follows:
- Advanced age;
- Smoking;
- Male gender;
- Diabetes;
- Hypertension;
- High blood fats and cholesterol levels;
- Irregular diet;
- Sedentary lifestyle;
What is the Importance of Arterial Occlusion?
Due to atherosclerosis, stenosis and occlusions occur in the leg arteries over the years. As a result, oxygen-rich clean blood cannot be delivered to the toes.
Although this situation does not cause significant complaints in the initial stage, as the degree of stenosis increases, leg pain, especially when walking, begins to appear. With the progression of the stenosis, the patient’s walking distance gradually decreases, and in the following periods, resting pain and finally foot wound and gangrene may develop. The picture that occurs in the last stage is called “Critical leg ischemia”.
For this reason, it is necessary to consult a doctor without losing time with the appearance of symptoms in peripheral arterial disease. With the diagnosis of the disease, the treatment to be applied is determined individually according to the degree of the disease and the complaints it causes.
However, with the diagnosis of peripheral artery disease, it is mandatory for the patient to quit smoking if he/she is a smoker. In cases of excessive alcohol consumption, alcohol consumption should be stopped or minimized. A healthy program in the diet should be adopted permanently. It is also very important for patients to exercise regularly and to reach their ideal weight for overweight patients.
Post-Treatment Considerations
Although the things to be considered after peripheral arterial disease may differ depending on the treatment applied, the determinant at this point is to follow the doctor’s recommendations for the patient.
Patients who are on bed rest for the first 24 hours following the treatment are kept under control despite the risk of developing a possible complication. In this process, they may need to take aspirin or anticoagulant drugs.
During the healing process, plenty of water should be consumed, heavy lifting should not be done for a few days, and the doctor’s recommendations should be followed completely for a healthy recovery process.